
03/17/2026
Crain’s New York Business: Health care interests take shape ahead of state budget negotiations

03/13/2026
News10 ABC: Lawmakers, Scientists Urge Governor for $100M in Biomedical Research

01/20/2026
AMSNY Awards 38 Medical School Scholarships to Strengthen New York’s Physician Workforce and Expand Access to Care

12/15/2025
Broad Coalition of Scientific, Healthcare, Higher Education and Other Organizations Calls on Governor Hochul to Establish New Institute to Ensure New York’s Global Leadership in Science and Biomedical Research Amid Changes in Federal Science Policies
05/15/2025
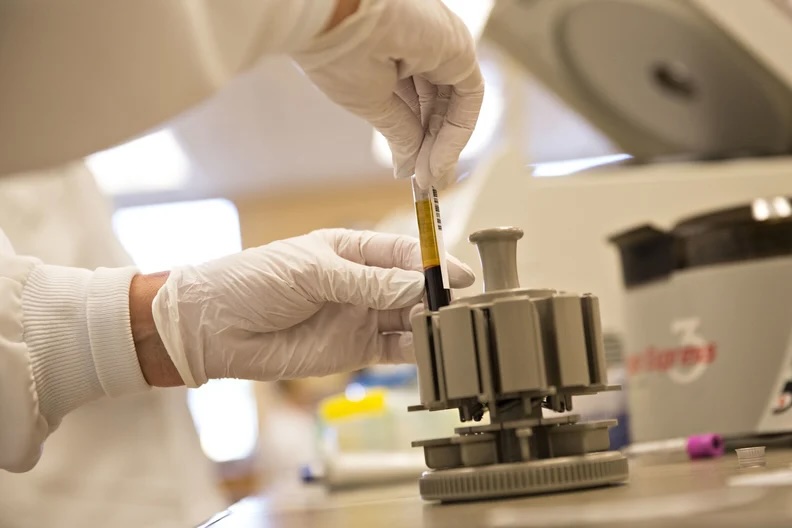
Crain’s New York Business Health Pulse: State invests in biomedical workforce as feds pull back funding

05/15/2025
AMSNY Statement: FY26 State Budget Boosts Medical Research, Programs and Scholarships for Students Pursuing Medical Education

04/29/2025
Jennifer Tassler Named to City & State’s “Who’s Who in Government” List
03/19/2025
NY1: AMSNY CEO on Potential Impact of Proposed Research Cut

03/19/2025
USA Today Network: Op-Ed by Jonathan Teyan on the Impact of Research Funding Cuts
03/06/2025
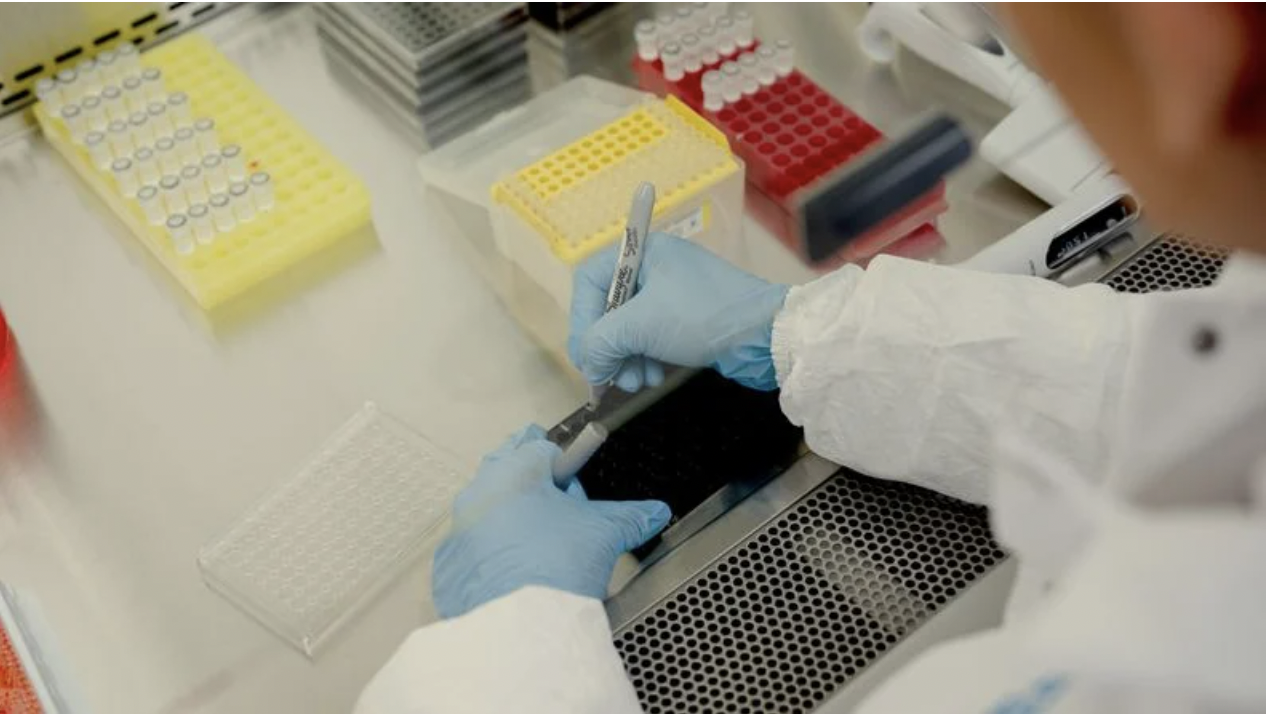
Crain’s New York: 30,000 New York jobs depend on shaky federal research funding

02/20/2025
Rochester Beacon: A direct attack on research funding

11/11/2024